The Federal Trade Commission (“FTC”) continues its investigation of Pharmacy Benefit Managers (“PBMs”) and their impact on prescription drug costs and availability. Last week, the FTC issued an interim report regarding its investigation.[1] Drug manufacturer rebates are one topic addressed by the FTC.
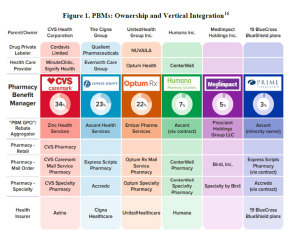
The FTC notes that the Big 3 PBMs (i.e., Caremark Rx, LLC, Express Scripts, Inc., and OptumRx, Inc.) all recently established separate, affiliated entities that they refer to as group purchasing organizations, or rebate aggregators. These entities negotiate rebates with drug manufacturers, a task that PBMs historically engaged in directly. See FTC Report p. 21. These entities, so called rebate aggregators, of the Big 3 PBMs are Ascent Health Services (affiliated with Express Scripts and Prime, and also serving Humana Pharmacy Solutions), Zinc Health Services (affiliated with CVS), and Emisar Pharma Services (affiliated with OptumRx) and they further obscure the flow of prescription drug money. Significantly, the FTC report reveals that rebate aggregators are cogs used to retain drug rebates for their own profit, rather than passing those savings on to self-funded employer plans (“Plans”) and other benefits providers that could use the savings to lower the cost of prescription drug coverage:
According to industry experts and members of Congress who have participated in hearings relating to PBM business practices, the PBMs may have spun off these rebate aggregators as separate entities for other purposes, such as to retain revenue from incremental fee structures. As a former OptumRx executive who helped establish Emisar explained, “[t]he intention of the G.P.O. [rebate aggregator] is to create a fee structure that can be retained and not passed on to a client.” Internal PBM documents appear to show novel methods of fee generation from these new rebate aggregators. One report estimates that since the PBMs spun off their rebate aggregators, they have extracted from drug manufacturers billions of dollars in additional fees, which doubled from $3.8 billion in 2018 to $7.6 billion in 2022.
FTC Report p. 22.
Per-member-per-month employee Plans have felt the rise in prescription drug costs and often wonder why their premiums rise year after year. In fact, members want answers for the rising cost of drugs and some members have even sued Plans for breach of fiduciary duties. That’s because Plans have a duty of prudence and a duty of loyalty to the members and must act in the members’ best interests. Thus, Plans must make sure that they understand their PBM contract, conduct diligence to ensure that the PBM is providing appropriate reimbursement – including an analysis of rebates and monies from drug manufacturers – and demand transparency. As shown in the FTC’s report, the current landscape of the PBM industry is complicated by vertical integration created by the PBMs (pictured below).
The first step in conducting due diligence and seeking transparency is to obtain the data and conduct audits of the PBM. The consequences of failing to audit PBMs extend beyond financial losses. Employers are entrusted with a significant responsibility: to manage employee benefits plans with diligence, prudence, and in the best interest of the participants. This fiduciary duty extends to all aspects of plan management, including the oversight of PBMs. PBMs play a pivotal role in controlling prescription drug costs, but without thorough audits, employers may unknowingly be subject to inflated charges, suboptimal terms, and practices that could be deemed as breaches of fiduciary duty by the employer. Legal ramifications, including class action lawsuits and breach of fiduciary claims, can damage a company’s reputation, erode employee trust, and result in significant legal costs.
How Frier Levitt Can Help
Frier Levitt represents self-funded employers in their dealings with PBMs. Our deep understanding of the legal landscape and PBM practices uniquely positions us to conduct comprehensive audits. We assess contract compliance, financial accuracy, and performance metrics to ensure that your PBM arrangements align with fiduciary standards and your company’s financial interests.
Don’t wait for a lawsuit to uncover deficiencies in your PBM management. Contact Frier Levitt today to learn how our PBM audit services can fortify your defense against fiduciary breach claims and secure the financial health of your employee benefits plan.
[1] The FTC’s report can be found at https://www.ftc.gov/system/files/ftc_gov/pdf/pharmacy-benefit-managers-staff-report.pdf.