Less than a month before David Joyner, president of CVS Caremark, testified under oath that Caremark passes through 100% of rebates, the State of Illinois executed a settlement with Caremark over wrongfully retained rebates. Self-funded plans must accept the facts – Pharmacy Benefit Managers (“PBMs”) do not pass through all rebates. Given that reality, Plans must be aware of substantial industry trends that impact plan obligations and liabilities. On June 24, 2024, CVS Caremark (“Caremark”) entered into a settlement agreement with the State of Illinois stemming from Caremark’s alleged wrongful retention of rebates. Caremark agreed to repay $45 million for pharmaceutical manufacturer rebates that Caremark or its affiliated rebate aggregator, Zinc Health Services, LLC (“Zinc”), failed to pass-through.
Caremark’s settlement comes on the heels of the Federal Trade Commission’s investigation and report on PBM contributions to inflating drug costs, the House Committee on Oversight and Accountability’s hearing and report on PBMs’ role in raising drug prices, and the Office of Personnel Management’s (“OPM”) investigation into Express Scripts, Inc (“ESI”). The OPM’s investigation into ESI found that ESI’s rebate aggregator, Ascent Health Services, LLC, retained approximately $16 million worth of rebates from a federal postal employee health plan. When PBMs deploy rebate schemes on governmental plans, it is obvious that self-funded commercial plans must audit their PBMs and protect themselves from the same schemes.
Why Do Manufacturers Pay Rebates?
Pharmaceutical manufacturers pay “money” to PBMs (typically through the PBM’s vertically integrated sister company, the “rebate aggregator”). PBMs “define” some of the manufacturer dollars as “rebates”. However, PBMs say that large amounts of money paid by manufactures are not “rebates”, but rather “data fees”, “price protection fees”, “communication fees” or some other arbitrary “fee”. Manufacturers pay rebates to encourage PBMs to place the manufacturer’s drug products on the Plan Sponsor’s PBM formulary. Manufacturers pay “more” to get their products placed on “preferred” formulary tiers, meaning patients pay less out of pocket to obtain the manufacturer’s product compared to drugs on non-preferred tiers and are therefore used more often by plan beneficiaries. Not being on “formulary” is the death knell for manufacturers; manufacturers pay dearly to stay alive.
How Are PBMs Able to Retain Manufacturer Rebates and Not Pass Through to Plans?
Rebate aggregators are vertically integrated with PBMs, meaning they are owned by the same parent company. PBMs actively conceal their use of rebate aggregators from plan clients. Thus, plans should look at their PBM contracts. What do PBMs reveal about aggregators? This allows the rebate aggregators to retain portions of rebates and other sham “fees”. PBMs pass only the “rebate” on to Plans (recall only some of the manufacturer money, according to PBMs, are “rebates”). According to the PBM, the retained rebate was not a “rebate” because in a secret contract it was arbitrarily “defined” as a different “fee”.
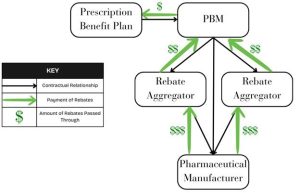
Manufacturer revenue intended for Self-funded plans are retained first by rebate aggregators and later by PBMs, as illustrated below:
Rebates retained by PBMs and/or rebate aggregators are substantial. It is critical that self-funded employers understand the relationship between PBMs and rebate aggregators, so that these relationships can be addressed when going through the RFP and contracting process with PBMs.
Caremark’s Settlement and Contracting with PBMs
Self-funded plan sponsors can avoid rebate schemes by fiercely negotiating the PBM contracts. Prohibiting rebate retention schemes comes down to two main provisions: (1) demanding disclosure of any subcontractors/affiliates the PBM utilizes as well as their expected compensation; and (2) the defining “rebate”. Demanding disclosure of rebate aggregator revenue is mandatory under the Employee Retirement Investment Security Act of 1974 (“ERISA”). ERISA obligates covered service providers, such as PBMs, to disclose all sources of direct and indirect compensation it or its subcontractors or affiliates will receive in exchange for providing services to an ERISA plan.[1] Armed with true financial disclosure, plans may audit PBM rebate retention. Of note, the same ERISA disclosure requirements apply to brokers or consultants that receive compensation from the PBM.
It’s All About the Definitions
Defining the term “rebate” is the single most important strategy to prevent rebate retention. PBMs carefully craft definitions with the intention to retain manufacturer funds—that are not “rebates” according to the PBM. These PBMs arbitrarily categorize a large percentage of manufacturer-paid dollars as an “administrative fee”, “data fee”, “communication fee” or some other illegitimate “fee”. By disguising rebates as “fees” through creative PBM contract definitions, PBMs retain rebates.
Plans must demand that all manufacturer derived revenue, regardless of how categorized by the PBM, is encompassed by the definition of rebate. To illustrate, the state of Illinois did exactly that as part of its settlement with Caremark, which stipulated that the definition of “rebate” in the State’s contract with Caremark effective July 1, 2024 would include “compensation of any …regardless of how categorized…”[2] The definition of rebate demanded by Illinois is all encompassing, and exemplifies the type of definition plan sponsors must negotiate into their agreements with PBMs to avoid falling victim to a rebate retention scheme.
What Should Plan Sponsors Do?
Plans must negotiate PBM contract provisions, especially the defined terms, and demand rebate transparency. Additionally, plan sponsors must audit their PBMs and, if necessary, take legal action. Of note, when conducting audits, plan sponsors must not rely upon brokers or consultants. As a plan fiduciary, ERISA obligates self-funded plan sponsors to manage benefits plans with diligence, prudence, and in the best interest of the plan and its beneficiaries. This fiduciary duty includes an obligation to effectively monitor PBMs. Failing to audit PBMs may lead to an employee allegation of breach of fiduciary duty. Frier Levitt is here to assist self-funded employers in navigating these complex waters, ensuring transparency, accountability, and fiduciary compliance in your PBM arrangements and help you recover rebates wrongfully retained by PBMs.
How Frier Levitt Can Help
Frier Levitt represents self-funded employers. We audit PBMs to assess contract compliance, financial accuracy, and performance metrics. Don’t wait for an employee lawsuit to uncover deficiencies in your PBM management.
[1] 29 U.S.C. § 1108(b)(2).
[2] Settlement Agreement between the State of Illinois and CaremarkPCS Health, LLC, 8 (executed June 24, 2024).