Plan sponsors and employers with self-funded employee health benefit plans are facing a new type of class action litigation risk. In late 2025, a string of class action lawsuits was filed by employees against companies that sponsor self-funded employee health benefit plans and the consultants and brokers that help administer various services and programs for those plans. The lawsuits allege that the plan sponsors breached their fiduciary obligations under the Employee Retirement Income Security Act of 1974 (ERISA) by allowing consultants/brokers to charge excessive fees and commissions for certain “voluntary benefits insurance” programs.
These lawsuits likely represent a new frontier of litigation that employers and plan sponsors may face moving into the new year. More importantly, they serve as a constant reminder that employers must remain vigilant in overseeing plan design and administration, including auditing and monitoring the fees and other revenues that third parties, like consultants and brokers, receive from plan assets. This article examines the allegations and legal theories asserted in two of these recent class action lawsuits.
Braham v. Lab. Corp. of America and Willis Towers Watson
The first of these lawsuits, filed in the U.S. District Court for the Northern District of Illinois, was brought by participants (individually and on behalf of a putative class) in the LabCorp Group Benefits Plan and its broker, Willis Towers Watson (WTW). The plaintiffs claim that the defendants failed to prudently manage the Plan’s “Voluntary Benefits Insurance” programs, allowing excessive participant premiums for accident, critical illness, and hospital indemnity insurance while receiving more than $14 million in broker commissions over six years. These voluntary benefits programs are often offered by brokers to plan sponsors to supplement existing benefits for their employees.
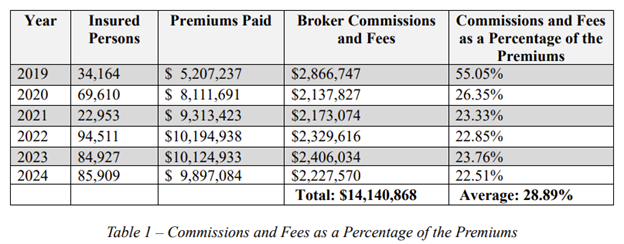
The plaintiffs argue that even for voluntary benefits, LabCorp and WTW remain fiduciaries to the Plan and therefore had a duty to monitor, negotiate, and prudently select insurance carriers, as well as ensure that the fees and commissions paid to brokers like WTW were reasonable. According to the complaint, the plaintiffs assert that LabCorp had no programs or policies in place to review, select, or monitor the insurance carriers’ services. LabCorp further paid excessive broker commissions and fees to WTW, representing a substantial portion of the total premiums paid for these programs, as shown in the table below:[1]
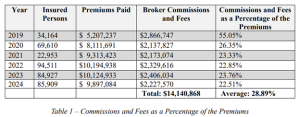
The complaint alleges that the average 28.89% in fees and commissions that LabCorp paid to WTW was higher than similar fee arrangement between WTW and other plans. For example, the complaint alleges, based on public reporting, that WTW collected 5% or less in commissions per year between 2020 and 2022 from Home Depot. Another company, Broadcom, paid as low as 2.6% in broker fees to WTW. These comparisons raise the question as to why LabCorp did not negotiate lower fees.
As further evidence of the “unreasonableness” of these commissions, the plaintiffs point to the low Medical Loss Ratio (MLR), which represents the proportion of premiums spent on actual clinical services and quality improvement as opposed to administrative expenses. Government programs like Medicare and Medicaid require that plans comply with a minimum MLR threshold of 85%. This means that, at minimum, 85% of premiums paid to the plan must be spent on clinical services and related costs. Other non-governmental plans also allegedly require MLRs ranging from 60% to 80%.
Using these MLRs as benchmarks, the plaintiffs allege that the true MLR for LabCorp’s Voluntary Benefits Insurance programs likely fell below 50%, since more than 28% of the premiums are going to broker commissions., It is inevitable that insurance carriers and other third parties will charge additional administrative and other fees on top of the broker fees.
Fellows v. Universal Services of America, Mercer Health, and Lockton Companies
The second lawsuit, filed in the Southern District of New York and brought by employees of Universal Services of America d/b/a Allied Universal, makes nearly identical allegations as the LabCorp complaint. Like the LabCorp case, the plaintiffs are a group of employees who are participants in the Allied Universal employee benefit plan, which allegedly used two brokers, Mercer and Lockton, and paid excess broker fees for Voluntary Benefits Insurance programs.
Plaintiffs included a similar “broker fees” table as in the LabCorp complaint, except here, Mercer and Lockton received more than $23 million in combined broker fees over six years. The average commission rate as a percentage of premiums, 39.80%, was also higher.[2]
Both complaints assert various causes of action including breach of fiduciary duty of prudence, failure to monitor fiduciaries, and prohibited transactions under ERISA, among others. As to relief, the complaints seek monetary recovery for losses, disgorgement of profits, equitable relief, removal of fiduciaries, plan reform, and attorneys’ fees.
A Potential Wave of Litigation Against Plans and Their Reliance on Brokers and Consultants
It is no secret that many sponsors of self-funded employee benefit plans rely on consultants, brokers, and coalitions to obtain insurance coverage for their beneficiaries. Consultants and brokers tout themselves as industry experts who know how to negotiate with Pharmacy Benefit Managers (PBMs), insurance carriers, and service providers on behalf of their plan clients. Indeed, many consultants like Lockton even administer RFPs on behalf of plans. However, the Braham and Fellows lawsuits demonstrate that plan sponsors must not assume that consultants and brokers will always act in the best interest of the plan. Over-reliance on these middlemen without adequate safeguards and monitoring will expose the plan to liability under ERISA.
Notably, Plaintiffs sued both the plan sponsor (LabCorp/Allied Universal) and the brokers (WTW, Mercer, Lockton). This is a departure from the ERISA lawsuits relating to mismanagement of pharmacy benefits, such as the cases against Johnson & Johnson, Wells Fargo, and JPMorgan Chase, where the plaintiffs only sued the employer/plan sponsor but not the PBMs that played a major role in the alleged ERISA breaches. The decision to include the brokers as defendants may be driven in part by (1) adverse court rulings granting motions to dismiss in favor of the plan sponsor defendants in those earlier cases because the PBM was not named as a defendant; and (2) the fact that brokers and consultants are subject to stringent disclosure requirements under the Consolidated Appropriations Act of 2021.
Frier Levitt is closely monitoring the development of these cases moving into 2026. It is highly likely that more plan sponsors will be named as defendants in similar lawsuits in the near future.
How Frier Levitt Can Help
Frier Levitt understands the legal landscape facing self-funded employer plans and routinely conducts audits on behalf of plan sponsors to ensure their service providers (including PBMs, TPAs, consultants and brokers) receive reasonable compensation in compliance with ERISA. We assess contract compliance, financial accuracy, and performance metrics to ensure your contracts align with fiduciary standards and your company’s financial interests. Proactive review can help identify potential issues before they result in litigation. Contact Frier Levitt today.
[1] See Braham et al. v. Lab. Corp. of America et al., N.D. Ill. 1:25-cv-15583, Doc. 1 at 29.
[2] See Fellows v. Universal Services of America LP et al., S.D.N.Y. 1:25-cv-10659, doc. 1, at 31.

Senior Associate

